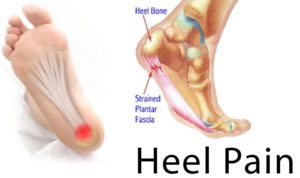
Heel pain is one of the most common conditions treated by podiatrists.
Our senior Podiatrist Fleur Fewster, has a special interest, along with extensive experience and success, in treating heel pain
Who gets heel pain?
The greatest incidence of heel pain is seen in middle-aged men and women. It is seen in those who take part in regular sporting activities, those who are significantly overweight and people who are on their feet a lot, particularly if they work on hard/concrete floors or if unsupportive footwear is worn.
It is thought that low arches, or feet that roll in too much (over pronation), or less commonly, rigid, highly arched feet and tight leg muscles are common contributors to heel pain.
These abnormal foot alignments can place too much stress on the soft tissues which attach to the heel bone( the plantar fascia or the achilles tendon).
Heel pain can sometimes result from an acute injury/soft tissue tear or bruise incurred while walking, running or jumping on hard surfaces.
Less commonly, heel pain can arise due to certain diseases such as inflammatory diseases.
Heel pain can also occur in children, usually between eight and thirteen, as they are growing fast and become increasingly active in sporting activities.
Plantar fasciitis
Plantar fasciitis is the most common condition that causes pain under the heel. Despite this it is often misdiagnosed, mistreated or sufferers are told they must put up with it until it goes away in a year or so!
Both heel pain and heel spurs are frequently associated with an inflammation of the long band of tissue ( ligament) that connect the heel and the ball of the foot. The inflammation of this ligament is called plantar fasciitis. It can be seen on an ultrasound or MRI scan.
Other causes of heel pain
-Strain of the achilles tendon attachment at the back of the heel
-An inflamed bursa (bursitis); a small, irritated sack of fluid at the back of the heel
-A neuroma ( a nerve growth) or a pinched nerve
-Haglund’s bumps, or ‘pump bumps’, a bony enlargement at the back of the heel bone
-Bruises or stress fractures to the heel bones.
Heel Spurs
One factor sometimes associated with heel pain is a heel spur, a bony growth under the heel bone.Heel spurs result from strain on soft tissues which attach to the heel bone.
It is now thought that spurs are not the main source of heel pain. Rather, the pain stems from the soft tissues pulling at their bony attachments, creating a spur. Many people are found to have heel spurs during general x-ray exams, yet they don’t suffer any heel pain. Surgical resection of spurs is now rare.
Your podiatrist may refer you for x-rays or an ultrasound to aid in the assessment of your feet and to help determine the source of the pain.
Overcoming the problem
What should you do?
If pain in or around your heels persists, you should limit excessive standing, walking or running, wear good quality, cushioned, lace up running or walking shoes as much as you can for support and consult an experienced podiatrist.
In most cases you do not need a Doctors referral to visit a private Podiatrist.
Treatment
Early treatment might involve specific stretching exercises, footwear advice, specialized taping or strapping and prescription of orthotic supports to wear in your shoes.
Some people may also benefit from short term use of anti-inflammatory medication and ice pack treatment. Taping/ strapping and orthotics can support the arch of the foot, reducing excessive strain of the painful and inflamed plantar fascia ligament which often rapidly reduces heel pain.
These treatments will effectively treat the majority of heel and arch pain, by addressing the cause, without the need for invasive treatments such as injections or surgery.
However some severe or unresponsive cases sometimes require a steroid or PPI injection (performed by a radiologist under ultrasound scan guidance) along with the above treatments, to help settle the condition.
In our practice less than 5 % of patients with heel pain go on to require these injections.
Only a relatively few cases of heel pain are referred by GPs for surgery. In our experience, surgery is very very rarely needed and this type of surgery is not always successful.
We would urge anyone suffering from heel pain to avoid surgery unless all other treatments above have been tried.
Recovery time
Your recovery will depend on the cause of your heel pain, your individual health and the type of treatment you receive. If you are suffering from plantar fasciitis/heel spur syndrome, in our experience, it generally takes between 1-3 months to substantially settle down, depending on how long you have had the problem, the type of treatment you have and your compliance with treatment advice.
Preventing Future Problems
Heel pain can settle down, but then later return. To avoid this recurrence, you may need to use supportive footwear and orthotic supports for the long term. Your Podiatrist can advise on your risk of future episodes and how to best avoid these.
-Footwear
Wear shoes that ” do up” such as lace up or velcro strap shoes. Buy shoes with cushioned/ shock-absorbent soles, and that hold the sides of your heel firmly in the shoe ( avoid thongs, scuffs or sling backs or super soft, bendy shoes like slippers) Avoid “dead flat” shoes like ballet flats, or soft canvas or mesh fashion shoes as these tend to be unsupportive and put more strain on the heel.
Do not wear shoes with excessive wear on the heels or soles.
-Future activity and Exercise
Once you have recovered, remember to prepare properly before exercising.
Warm-up before running or walking and do some stretching exercises afterwards. Wear the coreect shoes and supports recommended by your Podiatrist.
Pace yourself when you participate in athletic activities. If overweight, try walking along with non weight-bearing activities such as swimming or cycling.